The fibromyalgia story
Doctors had a problem
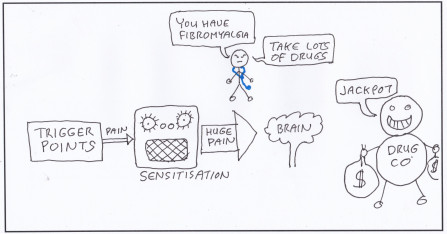
Years ago doctors had patients complaining of widespread pain, but could not find anything wrong. It is very un-doctor like to say they knew nothing so they made an impressive sounding word for it. They put in the diagnosis manual that if anyone had widespread pain for a while and the tests came back negative it was called "fibromyalgia".
Great for doctors and drug companies
This was a boon for doctors and drug companies (1,2)
- doctors got to sound authoritative even though they knew nothing
- specialists and testing laboratories make a fortune "diagnosing" this condition
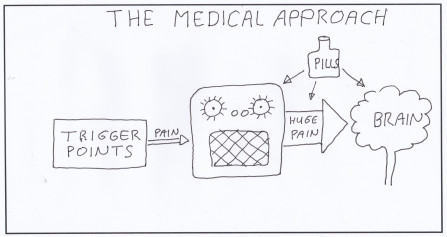
- drug companies are happily selling symptom relieving drugs to patients who will never get better
Solution? No way,, that would spoil everything
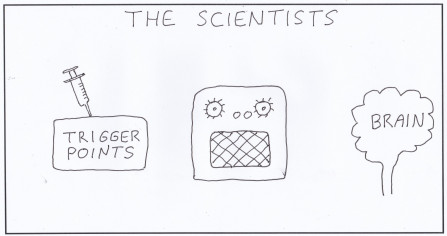
Then, over a decade ago several scientists worked out what causes fibromyalgia and even successfully treated it, but it takes a while for such knowledge to get through to doctors. For example, it took 14 years from when Penicillin was discovered to when doctors started using it. In the case of the fibromyalgia doctors and drug companies are on a good thing, so they are in no hurry. In this article we'll share with you what the scientists found and what you can do.