An easy safe way to improve sleep quality while reducing anxiety, heart rate and blood pressure
A recent study published in the journal Asian Pacific Journal of Cancer Prevention showed that a simple 15 minute back massage each day... Read Article

If you suffer from shoulder pain that won't go away you're not alone. Studies show that only 21% of sufferers are better after 6 months. The reason shoulder pain won't go away is because as clinical trials show:
In this article we'll go over the causes and effective therapy that get overlooked. The main thing though is to provide the best possible resource to help you get better. To do this we'll give you some practical advice plus show you as much self therapy as possible. You may need some professional help though. If you do we’ll give you enough information to find a suitable professional and discuss things in an informed manner.
Overlooked cause one: (myofascial) trigger points
Overlooked cause two: head and shoulders forward posture
Overlooked effective therapy: trigger point therapy
What’s wrong with typical shoulder therapy
Practical advice to help your shoulder pain
The first overlooked cause of shoulder pain is (myofascial) trigger points, which are those tender lumps in your muscles that therapists find. As shown below, trigger points cause shoulder pain:
Trigger points are those tender lumps in muscles that massage therapists find. For more info please see our article Trigger point basics, but the key issues are that trigger points:
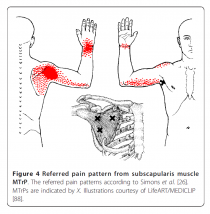
Trigger points directly cause shoulder pain by shooting referred pain. Scientists have mapped where trigger points refer pain to. This diagram is one of one of many muscles that shoot pain to the shoulder (1,2).
Trigger points indirectly cause shoulder pain by tightening muscles and stopping them working properly. This affects the movement of the shoulder joint, potentially causing abnormal stress and pinching (called “impingement syndrome”). Let's share how this happens.
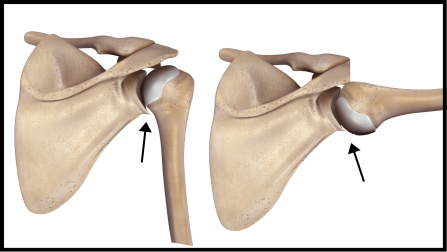
As this picture shows your shoulder joint has a large rounded surface sitting in a shallow socket. As you lift your arm the large rounded surface needs to rotate and slide down so:
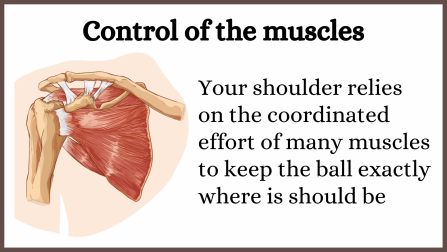
With a large ball sitting in such a shallow socket it is fairly unstable, so without guidance it would easily slop around and cause damage. As this diagram shows you have a team of short muscles that hold the rounded surface in the best position. The key is that these muscles need to be able to work as a well coordinated team to keep the rounded surface exactly where it should be. However, as discussed in a separate article, with trigger points causing muscles to be abnormally tight and not work properly joint movement becomes coordinated, and this cause several problems.
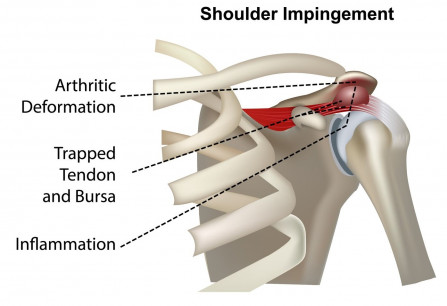
Uncoordinated shoulder joint movement is the major cause of the commonly diagnosed “impingement syndrome”. When “sitting” normally there is plenty of space above the joint for the critical structures. However, if the position of the rounded part is moved just slightly it causes it to impinge on those structures.
The pressure is no longer evenly spread across the joint surfaces so the joints wear faster. Long term this causes degenerative or arthritic changes that can be seen on x/ray.
When your shoulder joint is moving abnormally parts often have to compensate or work in ways they were not designed to and become over-stressed. Over time these can become painful or are easily injured.
As shown by several studies (3-8), the second overlooked cause of shoulder pain is a head forward posture. This alters the angle that the arm hangs and the direction the shoulder joint moves, which puts a lot of abnormal strain on some parts, and causes others to jamb together when they otherwise would move freely.
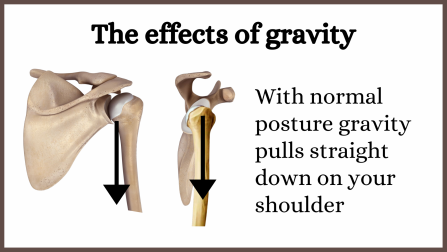
As shown in this diagram your arm usually hangs straight down roughly in line with your shoulder blade. This creates the best gap above for those sensitive structured discussed above, and also the best position for the supporting muscles and tissues.

This pic shows a diagram of head forward posture from one of the scientific studies. As the diagram next to it shows this cause the shoulder blade to be angled forward. With the arm still hanging straight down this alters the angle of the joint, placing unusual stress on the muscles and tissues and making structures more likely to pinch.
Trigger points are a major overlooked cause of shoulder pain so it should come as no surprise that treating trigger points is a major overlooked therapy. Trigger point therapy is a very very effective therapy that has been successfully used in many clinical trials. Scientists agree, with one scientific review of 16 studies into shoulder pain stating that trigger points were the most common cause and their treatment should be the number one priority (9). Further, another researcher stated that if trigger points were not taken into consideration they could perpetuate and aggravate the problem, hindering diagnosis and making the applied treatments ineffective (10).

Apart from being completely obvious, as you can see in the appendix below, there is a massive amount of scientific research confirming these causes and that treating trigger points should be the first consideration. However, as shown in these three typical medical journal articles (11–13) medical journals usually fail to mention these issues . Instead doctors are advised to use drugs and therapies that don’t work. This omission is easy to understand when you appreciate that most sources of information for doctors rely on drug company funds. If you don’t get better they sell more drugs.
The main purpose of this article is to give you the best resource possible to help your shoulder get better. To do this we'll:
The issues that medics tend to look at such as inflammation, impingement and damage seen on scans are often secondary to the abnormal stresses from the functional and postural issues discussed above. However, these secondary effects are too often treated completely oblivious to their cause.
While exercises are often prescribed to help shoulder pain, studies show that they are of little help and can often worsen the problem. The reason is very simple. As discussed in our article functional rehabilitation and demonstrated in several studies of shoulder function, exercises cannot correct the abnormal function caused by trigger points or abnormal posture. When the exercises are done your body uses that same abnormal mechanics that causes the problem in the first place, and likely accelerates any damage.
Our goal is to give you the best possible resource to help your shoulder pain. We’ve made you aware of some common miss-information and potential pit falls. Now we’ll give you some positive steps. Please keep in mind that we cannot give specific information to those we have not personally examined so consider this as general information to be discussed with a professional familiar with your own needs.
Trigger points were found to be a major cause of shoulder pain, and several clinical trials showed that treating the trigger points can give excellent relief (2,9,14–18). We have a comprehensive guide called Massage and trigger point therapy for shoulder pain: with self help options that gives:
If you know of any activities that are aggravating your condition stop doing them, at least temporarily while your shoulder settles down. This includes any exercises you may have been prescribed.
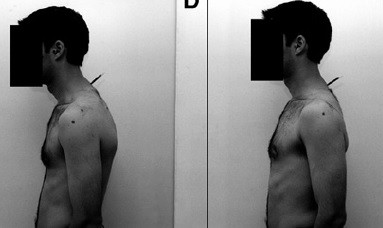
As discussed above a head and shoulder forward posture will create abnormal stress on your shoulder joints. If you have this condition it needs to be fixed. This diagram shows you what we mean by a head and shoulders forward posture. The person on the left has his head and shoulders forward, while on the right his head and shoulders are (almost) nicely balanced.
If you do have a head and shoulders forward posture, just like shoulder remedies a lot of the medical solutions such as exercises, taping, braces and advice are ill-conceived and ineffective. Please see this article for information about these spinal problems and how they are fixed.
There are often issues within the shoulder and other joints that inhibit them from working normally. The simplest way to think of these is as adhesions or restrictions stopping the joint surfaces from sliding across each other. Please see this article for more information about these and how they are treated.
There are many possible medical causes of shoulder pain that could be considered, especially if the pain is severe or not settling using conservative measures. Some are listed below. Please keep in mind that some may be secondary and will resolve once any abnormal stress is removed, but they may also be:
We realise that the contents of this article are contrary to information provided by medical journals and respected professionals, so we conclude with documentation of the research papers and clinical trials that support the major points.
We are continually adding more information on research and uses. Subscribe below to have us email them to you "hot off the press".

Several years ago Dr Graeme, a Chiropractor practicing in Victoria, Australia was looking for a serious hand held massager his patients could use at home to get the extra quality massage they needed. The ones he found in the shops and on-line for home use looked nice but were not serious, and... read more
A recent study published in the journal Asian Pacific Journal of Cancer Prevention showed that a simple 15 minute back massage each day... Read Article
Most movements require the co-ordinated contraction and relaxation of numerous muscles. The neurological control of this is known as a... Read Article
A gimmick is something that is not of real value used to attract attention, usually to get you to buy something. Massager guns certainly... Read Article
Although often described as “misaligned vertebrae” or “bones out of place” most issues that cause back pain actually involve abnormal... Read Article
As practitioners we are continually dealing with dysfunctional musculoskeletal systems. Typically dysfunction develops and is perpetuated... Read Article
Using a hand held massager is simple. You place the vibrating head on the muscle, making good contact, and allow the vibrations to... Read Article
Massage therapy has been shown by clinical trials to be an excellent therapy for fibromyalgia. This is because the muscular problems... Read Article
Clinical trials have proven that regular massages are very effective in preventing and reducing pain (see table below). The best example... Read Article
Do not refresh or leave this page until loading complete.